
Our study indicates that clinicians need to be focusing on ways to improve body composition, rather than on BMI alone, when counseling older adults on preventative health behaviors.” So many studies on the mortality impact of obesity focus on BMI. Preethi Srikanthan, one of the study’s authors, states, “As there is no gold-standard measure of body composition, several studies have addressed this question using different measurement techniques and have obtained different results. Higher muscle mass was correlated with lower mortality, suggesting that medical professionals should focus special energy on assessment of lean body mass, favoring more detailed measures over BMI.ĭr.


One study found that muscle mass, rather than total body mass index, was a better predictor of mortality in older adults. New studies echo the importance of lean mass analysis in older adults. Moreover, even in younger adults, monitoring lean mass is important for taking preventative action against sarcopenia. It is important that medical professionals assess older adults’ lean mass to provide effective treatment for this prevalent condition. To date, exercise and nutrition are the most effective treatments in combating sarcopenia. Consequences of sarcopenia can be devastating, and include disability, loss of function, frailty, chronic disease, and consequently, mortality. As part of the organic aging process, sarcopenia affects virtually every older adult. Monitoring lean mass, while important in the younger years, is more salient as we age, when skeletal muscle mass that is key for functionality declines in a condition called sarcopenia. Lean mass is particularly relevant to older adults. Studies such as these indicate that health professionals should look to measures beyond BMI to provide a more accurate account of body weight status, especially when lean mass is a measure of interest. These findings suggest that a high body mass index may often be the result of higher muscle density, which is actually beneficial to health. Moreover, the study showed that although BMI was positively correlated with body fat, it had a higher correlation with lean body mass.
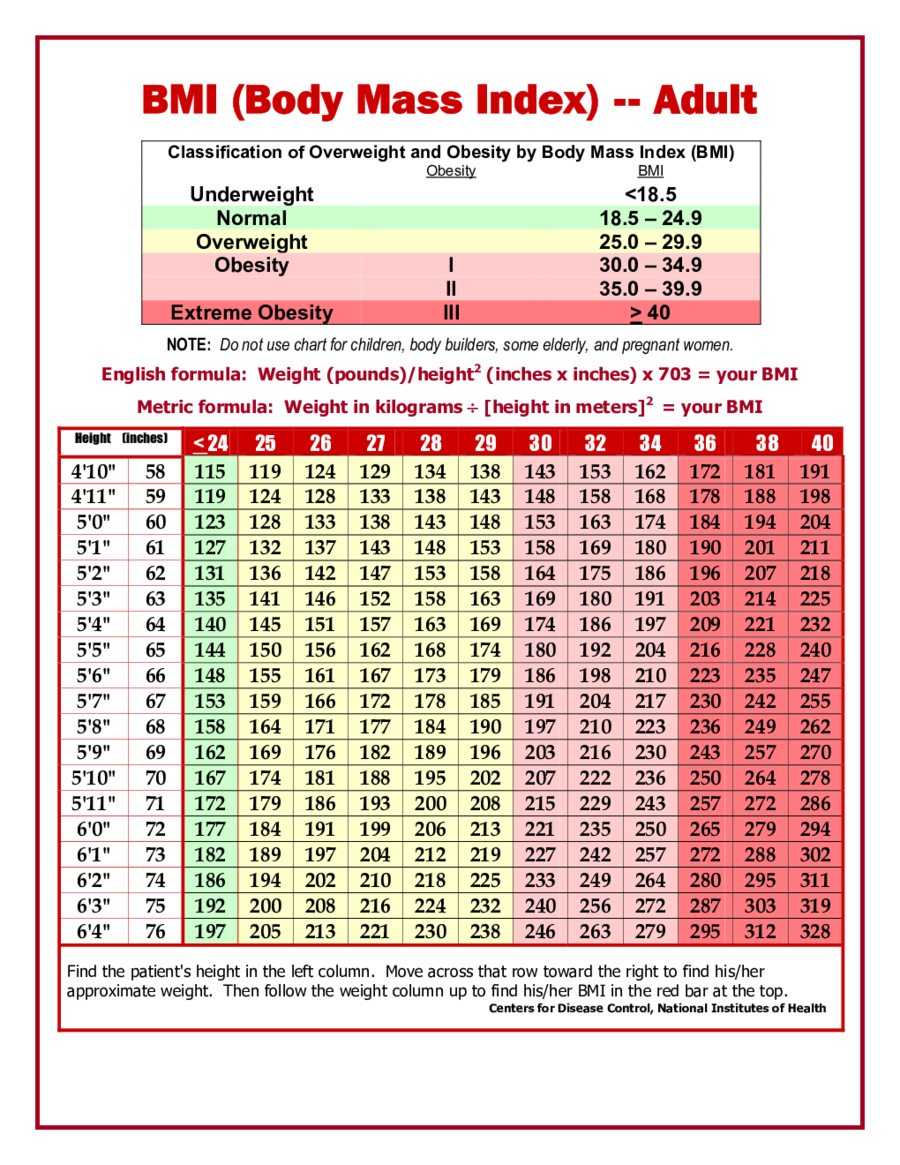
A recent study found that in 41% of patients, BMI mislabeled body fat status. Consequently, BMI may miscategorize patients. Weight, as a measure, lumps fat mass and lean mass into a single number, failing to distinguish between the two. As might be supposed, this measure does not always provide an accurate account of body composition. It may be prudent to consider different weigh status measures for older adults, especially on an individual basis, to account for age-related changes in body composition.īMI is calculated by taking an individual’s weight (in kilograms) divided by height squared (in meters). Furthermore, assessing lean mass in older individuals is crucial-maintaining lean mass is important for functionality and overall health in the older years. Loss of lean mass may be the culprit behind the lower BMI’s observed in older adults. BMI, while convenient for large sample sizes, does not distinguish between fat mass and lean mass, the latter typically diminishing as we age. Why might this be the case? Are older adults adopting better lifestyle habits? Is it easier to maintain a healthy body weight as one ages? Actually, research suggests these numbers may be misleading. Many trends in the Sightlines data on BMI merit investigation, one of which is the finding that Americans in the oldest age group (adults 75+) are most likely to have healthy BMI’s. Because of its relevance to longevity, weight status is a key measure in the Sightlines project. Body mass index, or BMI, is a common weight-for-height measure used to classify individuals by weight status-as underweight, normal weight, overweight, or obese.
